What is 'water on the knee'?
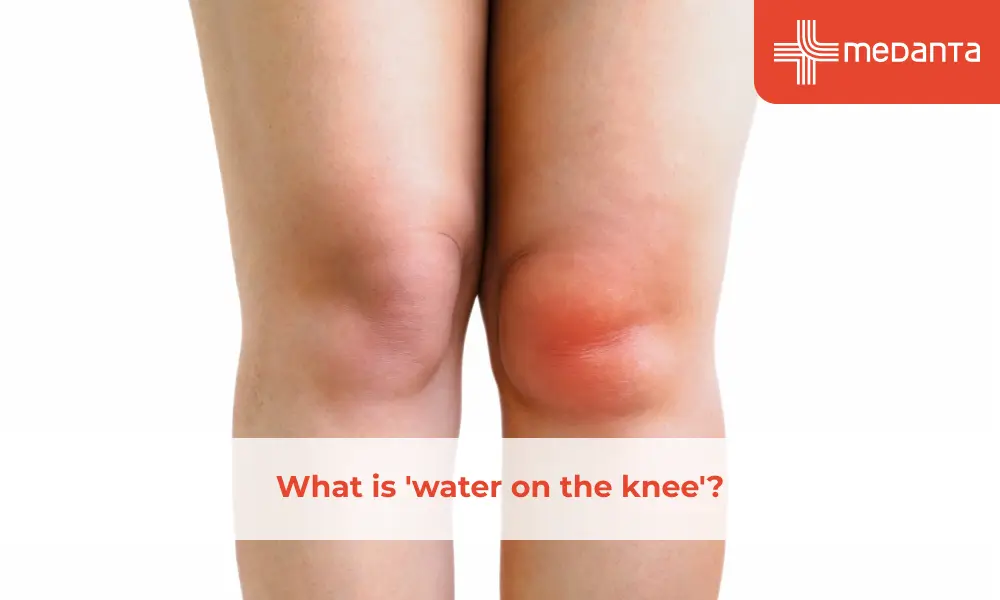
A small amount of fluid exists within all of the joints in the body in order to keep them lubricated and supple. When you injure your knee or are in the process of recovering from a health condition such as arthritis, your body may sometimes produce an excess amount of fluid to protect your knee. This is called 'knee effusion' or 'water on the knee'.
You will know if there is fluid build-up around your knee simply by the way it looks: one knee may seem more swollen and puffy than the other. Your finger may leave an indent when you press on the swollen knee, or it may be warm to touch. This may also be associated with mild to severe knee pain when walking, and the inability to bend or flex your knee, or fold or straighten your leg without significant pain or discomfort.
Self-care for swollen knee or knee effusion
-
Rest your knee as much as possible, use cushions for support.
-
Prescription Painkillers can help, or gently massage with pain-relieving gel.
-
Alternate between using hot and cold compresses to relieve your swelling and pain.
-
If you are an athlete, choose other low-impact exercises and take a break from strenuous knee activities for a few days.
-
Consider taking supplements like glucosamine or ginger that can help with the pain. Do check with your doctor if you could have any allergies to the ingredients beforehand.
-
Keep your knee and joints moving to avoid joint and muscle stiffness which could worsen your pain.
Despite these self-management measures, if your symptoms last for over three days and you develop a high fever, or if your knee pain is unbearable and you feel like it will 'give way', you must consult a doctor soon.
What are the likely causes of knee effusion, and what are its effects?
The 'water on the knee' condition could be caused by a variety of risk factors. For example, it could be due to your age and how prone you are to arthritis or it could be related to your weight if you are obese.
Knee effusion is commonly also injury-related, such as, if you have had a torn ligament or cartilage, or a recent fracture. Fluid retention in the knee could be the result of an infection caused by your recent injury, or it could be due to pre-existing conditions such as:
-
Rheumatoid Arthritis
-
Gout
-
Bursitis, and Septic bursitis
-
Osteoarthritis
-
Reactive arthritis
-
Septic arthritis
-
Tumours or Cysts
Whatever the cause, it is advisable to get your swollen knee diagnosed and treated appropriately. A delay in treatment could lead to further pain and complications such as weakness or loss of muscle in the thigh or atrophy. An unchecked swelling in the knee may also lead to painful fluid build-up: a condition called 'baker's cyst', where the fluid then has to be surgically removed.
Diagnosis and Treatment
In order to ascertain the exact cause of excess fluid in your knee, your doctor may conduct an imaging test or a combination of tests such as an X-Ray, Ultrasound scan or MRI scan. These scans will rule out the risks associated with broken or dislocated bones or fractures, arthritis or ligament- or tissue-related injuries.
Arthrocentesis
Following the scans, your doctor may want to conduct an 'arthrocentisis' or 'joint aspiration' of the knee, in which case the fluid from your knee is extracted and checked for traces of blood, indicating an internal injury; uric acid crystals which could mean pseudogout or gout; and pus and bacteria, which point to infection.
The diagnosis of the fluid in the knee determines the kind of treatment suitable for it. For an infection-related swelling, for example, your doctor will prescribe antibiotics. You may also be advised to take over-the-counter pain medication for the inflammation, or stronger corticosteroids such as prednisone for immediate, short-term pain relief.
Arthroscopy
Following the arthrocentesis, your doctor may also conduct a procedure called arthroscopy: a small incision is made to the knee through which a lighted tube is inserted into your knee joint. The tool called an arthroscope, is designed to remove damaged loose tissue and repair the knee.
Surgery
Despite the preliminary measures discussed above, if your knee pain is unbearable and the knee cannot take your weight, the doctor may recommend that you consider joint replacement or knee replacement surgery to fix your condition.






