Things You Must Know About Prostate Cancer
Globally, prostate cancer is the second most frequently diagnosed cancer and the fifth most common cause of cancer death among men. Its incidence has particularly increased after 1991 with the advent of prostate-specific antigen (PSA) screening in men over 50 years of age. Most cases present after the age of 60 years. Risk factors include older age, family history, race (Caucasians).
Prostate cancer rarely causes symptoms at an early stage. The presence of symptoms suggests a locally advanced or metastatic disease. Common manifestations of locally advanced prostate cancer include obstructive urinary symptoms, ureteral obstruction causing renal failure. Manifestations of metastatic disease include bone pain, pathologic fractures, anemia, and lower extremity edema. Timely detection of prostate cancer and its effective treatment leads to excellent outcomes and survival.
Suspicion of prostate cancer arises when men present with the above-mentioned symptoms/ raised PSA levels/ abnormal digital rectal examination. Confirmation of the diagnosis is done by TRUS guided prostate biopsy. Newer modalities of MR-fusion biopsies are also available for highly suspected prostate cancers with negative biopsies or tumors in difficult to access locations. After diagnosis, staging is done via a PSMA PET scan/bone scan to decide for options of treatment.
There are multiple treatment modalities depending on stage, grade, PSA levels, and life expectancy of patients. After staging, prostate cancer is classified into localized, locally advanced, and metastatic disease.
Localized low-risk prostate cancer can be managed by active surveillance or watchful waiting with the intent for regular monitoring and active intervention if required. These patients should also be offered definitive local therapies with curative intent (surgery and radiotherapy).
Robot-assisted radical prostatectomy is now considered the gold standard treatment for localized as well as highly selective locally advanced disease patients. Robotic prostatectomy is associated with a significantly lower transfusion rate and shorter hospital stay compared to open radical prostatectomy. Metastatic prostate cancer patients can be treated with hormonal therapy, chemotherapy, or surgical castration. These methods have been found to prolong cancer-specific survival and improve quality of life. These patients also require bone-strengthening drugs to reduce skeletal-related events as bone metastases is the earliest to manifest in these patients. Newer modalities include immunotherapy and radiopharmaceuticals.
Various effective treatment modalities have emerged which have led to cure in early stage disease, improvement in overall survival and quality of life in late stage diseases. Medanta is at the forefront of diagnosing and treating prostate cancer with an experienced team of doctors supported by cutting-edge technology.

Case Study
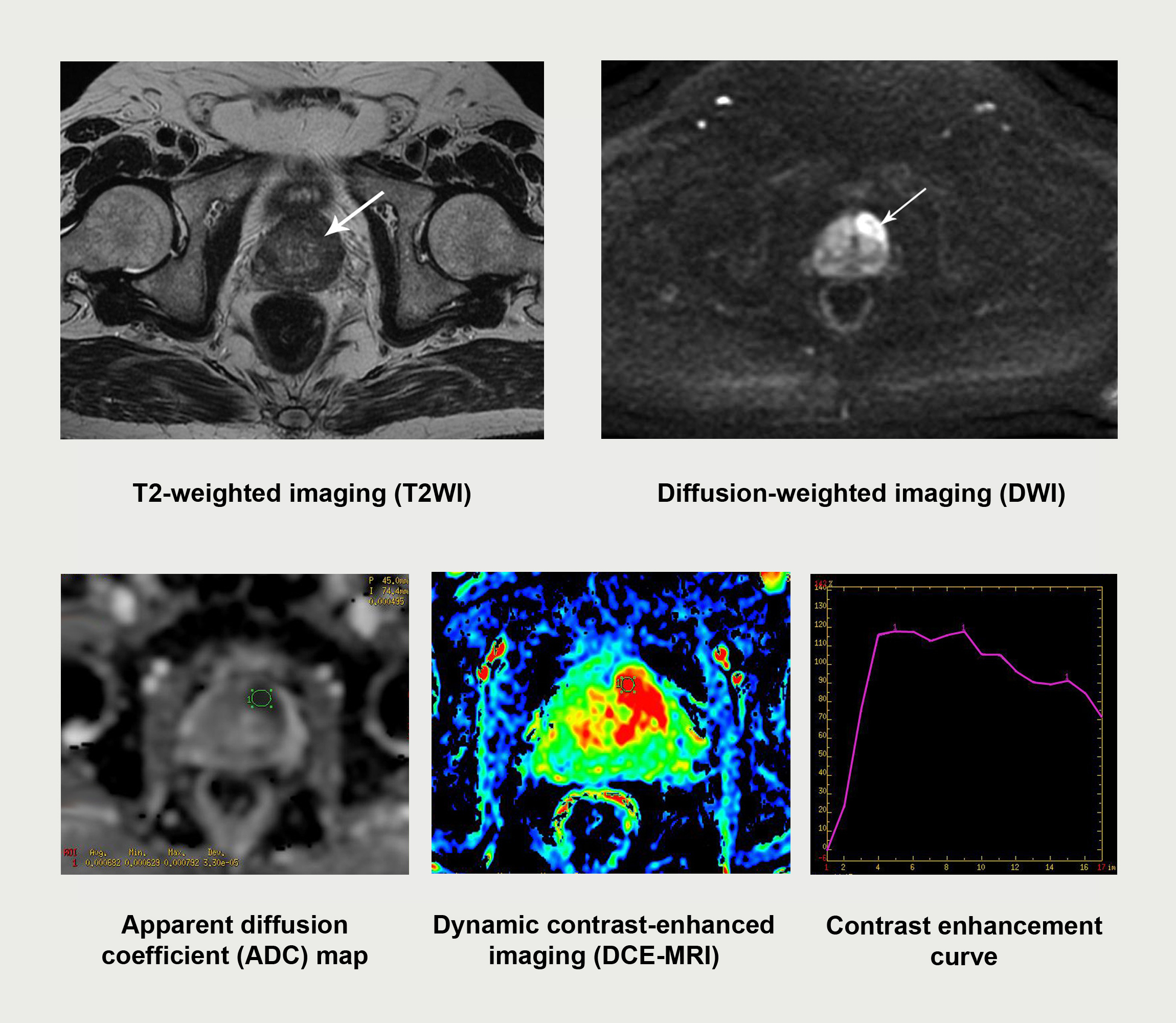
A 63-year-old male patient was referred to Medanta for elevated PSA and a negative prostate biopsy. His PSA was 11.3 but his ultrasound guided prostate biopsy did not reveal any cancer tissue. Dynamic MRI of prostate was done which showed a suspicious lesion in the anterior part of the prostate, a location not easy to target with just an ultrasound guided biopsy.
State-of-the-art 3D Artemis semi-robotic prostate fusion biopsy system was used to precisely target the suspicious part of the gland. The report came positive with high-risk prostate cancer. PSMA PET CT scan was done for distant staging. The patient was offered curative treatment options in the form of Robot Assisted Radical Prostatectomy (RARP) and Radical Radiotherapy. He opted for RARP.
The minimally invasive surgery was done using the DaVinci robotic system. The patient was very comfortable post surgery and was able to get out of bed, sit on a chair and have food the same evening. He was discharged within 48 hours of surgery. Within three months, he was fully continent and actively participating in the penile rehabilitation program for faster recovery of erectile function. The patient is cancer-free one year post-surgery and enjoying healthy life.