THE EXCHANGE | Newsletter October 2020
Medanta Brings World-Class Affordable Healthcare to Patna
In continuation of its commitment to medical excellence and patient care, Medanta launched Jaiprabha Medanta Super Specialty Hospital in Patna. Expected to be operational shortly, it will complement the flagship Medanta Hospital at Gurugram in the New Delhi National Capital Region.

The state-of-the-art hospital will comprise the following specialties and services: cardiology and cardiac surgery, neurology, gastroenterology, urology, nephrology, orthopaedics, radiology, transfusion medicine, pulmonary medicine, medical oncology, internal medicine, endocrinology, hepatology, transplant and critical care among others. 500-bed Jaiprabha Medanta Super Specialty Hospital is a clinical unit with an integrated holistic design building.

Medanta is a combination of medical expertise, cutting-edge technology, and state-of-the-art infrastructure with a highly integrated information system. With an outstanding pool of doctors and clinical researchers, Medanta continually fosters cohort-driven, multi-disciplinary approach to treatment, inspiring new ideas and translating scientific advances into industry best practices. Its philosophy of healthcare delivery is to integrate modern and traditional forms of medicine in order to provide accessible and affordable healthcare.

Dr Naresh Trehan
Chairman and
Managing Director – Medanta
Medanta is envisioned as a blend of best technology and treatment. It will bring world-class healthcare to Bihar at an affordable price. People of the state and the surrounding areas will be able to access these services with convenience and will no longer have to travel long distances to get best medical care.
Medanta’s Expertise
Soft Tissue Tumours
Not uncommon, soft tissue tumours arise anywhere in the soft tissues of the body i.e. muscle, tendon, fat, lymphatics, nerves and wall of blood vessels. These tumours are mostly found on arms, legs, chest and abdominal wall. These can be benign (non-cancerous) or malignant. The malignant ones are called sarcomas.
While the non-cancerous soft tissue tumours are treated by surgery alone, most soft tissue sarcomas are treated by a team of specialists comprising surgeon, radiation oncologist, medical oncologist and reconstructive surgeon. At Medanta, customized treatment for every patient is offered by the Disease Management Group which has all the above mentioned super specialists who discusses each case and prescribe the most suitable line of treatment complemented by state-of-the-art technology and world-class infrastructure.
Case Study
A 14-year-old female presented with pain and small mass in the right hip since 2-3 months. The mass had increased in size insidiously from 4 cm in diameter to about the 10 cm in the same duration. She also complained of intermittent excruciating pain radiating from back of the hip to back of the knee which would reduce by taking medication (Gabapentin), fever accompanied by generalized body ache, and a history of weight loss accompanied by loss of appetite. Examination revealed a palpable mass in the right hip and upper thigh approximately 9x10 cms in size, with mild tenderness but no overlying skin changes.
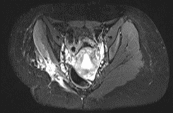
Parents had consulted another cancer centre where FNAC done was suggestive of spindle cell neoplasm. Immunohistochemistry (IHC) of the tumor cells suggested Synovial Sarcoma. MRI of both hip joints done there was suggestive of large well-defined intramuscular mixed intensity lesion with heterogenous enhancement seen in right gluteus maximus measuring 9.7 x 7.2 x 6.5 cm.
The patient came to Medanta on August 2016 and her further treatment continued here. She underwent whole body PET scan which was also suggestive of a large well defined lesion showing heterogenous enhancement and appearing largely isodense with the surrounding muscle. It also showed areas of internal necrosis and intense peripheral hypermetabolism (SUVmax 10.87). Overlying skin and subcutaneous tissue was normal. There was no evidence of erosion /destruction of underlying bones. The right hip joint space was maintained with no evidence of any intraarticular extension of the mass. No associated metastasis was observed.
Bone marrow aspirate showed signs of cellular arrow with no abnormal cells. The histopathology block submitted from the other cancer centre was reviewed and was reported as cellular tissue composed of a hemorrhagic background with large monolayered sheets of spindle shaped cells running in fascicles, cells have spindle shaped nuclei with blunted ends. The cells had moderately eosinophilic cytoplasm. Few round cells with a rim of cytoplasm and round vesicular nuclei were evident.
No evidence of necrosis or mitotic figures was present; consistent with a mesenchymal lesion (Spindle / Biphasic cells). The cytopathology and immunohistochemistry report done was suggestive of low grade sarcoma favouring low-grade fibrosarcoma.
The Disease Management Group did not recommend upfront resection in view of soft tissue extension of the mass and prescribed radiotherapy and chemotherapy to shrink the mass in order to make it more resectable. As part of treatment, the patient received Inj Vincristine, and was subsequently planned for neoadjuvant Radiation therapy (VMAT). She received 5040cGy in 28Fractions to tumor bed followed by surgical excision with clear margins with high-dose rate brachytherapy.
Four years post-treatment, the patient is on regular follow up and is free of disease.
medanta.org/dr-rajeev-agarwal/
medanta.org/dr-satya-prakash-yadav/
medanta.org/dr-tejinder-kataria/
Expanding the Scope and Safety of Pancreatic Surgery in India
Though the incidence of periampullary and pancreatic tumours in India is low compared to west, they have been rising over the past decade. That has caused a higher number of patients to seek pancreatic surgery, which has a notorious reputation of not just being complicated, but also highly morbid. Surgery remains the main modality of treatment in pancreatic tumors and is often the first. Ensuring safety and improving outcomes following pancreatic surgery, is therefore, of paramount importance. Dr Adarsh Chaudhary, Chairman - GI Surgery, GI Oncology and Bariatric Surgery, Institute of Digestive and Hepatobiliary Sciences shares how this has changed over the last few years.
Introducing enhanced recovery protocols
Enhanced recovery protocols have been a part of surgical practice for some time now, but acceptance for major procedures like pancreatectomies has been slow. With over 100 pancreatectomies being performed every year, we have been able to establish ERAS for pancreatic surgery at Medanta. This has decreased the mean postoperative hospital stay by two days in patients who undergo Whipple’s procedure, with over two-third patients getting discharged within fifth to seventh postoperative day. Protocol based
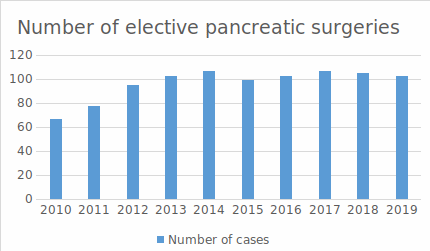
care decreases ambiguity of treatment and helps in early identification of complications and timely interventions.Decreasing morbidity following pancreatic surgery
Pancreatic surgery is widely feared of, because of a high post-operative morbidity rate of 30-40%. The two most feared complications are postop pancreatic fistulae and bleeding. Studies have shown that surgery in high volume centers significantly decrease complication and mortality rates. Post-operative outcomes at Medanta match world standard, with a low rate of clinically relevant pancreatic fistula and an extremely low rate of re-explorations.
Complex resections
Large tumours, especially those requiring venous resection are best managed at high volume centers. These tumours often benefit from pre-operative chemo-radiotherapy and multi-disciplinary approach. About 10-15% of operative work at Medanta comprises patients who have received pre-operative therapy and benefit from surgical resection of their disease thereby.
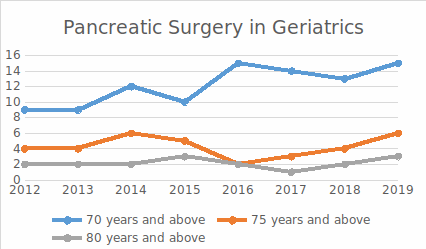
Increasing number of geriatric patients
Pancreatic cancers are typically said to occur beyond the sixth decade of life. That goes to suggest that most patients being offered surgery would be elderly, to broadly state it. In the last few years, the number of geriatric patients being operated at Medanta have been increasing, with even octogenarians being offered definitive surgery. It has been realized that physiological age and comorbid status of the patient are more important that the chronological age of the patient. And in our experience, most of these patients do extremely well and benefit from surgical intervention.
Multi-disciplinary approach
The role played by our gastroenterologists, radiologists and critical care experts cannot be emphasized enough. With dedicated GI critical care teams and intervention radiology support, we have been able to increase patient salvage rates at Medanta by mitigating the burden of major complications.
(With inputs from Dr Deeksha Kapoor
medanta.org/dr-adarsh-chaudhary/
Cancer Outlook in India
Recent National Cancer Registry Programme report released by the Indian Council of Medical Research (ICMR) and the National Centre for Disease Informatics & Research (NCDIR) provides a comprehensive overview of data on the patterns of cancer, leading sites, trends and burden, cancer incidence and treatment offered by the most prominent sites of cancer care in India. The data collected is useful in developing strategies for prevention, control and better care. These estimates are based on information collected from 28 Population Based Cancer Registries (PBCRs) and 58 Hospital Based Cancer Registries (HBCRs). As a HBCR, Medanta has been an integral part of the National Cancer Registry for the last ten years. Dr Tejinder Kataria, Chairperson, Radiation Oncology, Medanta - Gurugram shares broad contours of the recent report.
ICMR-NCDIR National Cancer Registry Programme estimates 12% increase in cancer cases in the country by 2025. Tobacco related cancers are estimated to contribute 4.2 lac (27.2%) of the total cancer burden. Breast cancer will be the most common cancer in women with an estimated number of 2.3 lac (14.8%) cases followed by cervical cancer. Gastrointestinal tract cancer for both genders is estimated to contribute 3.1 lakhs (19.8%).
Delhi PBCR reported 31,032 cases in males and 29,065 in females for the period 2012-2014. Age adjusted incidence rate (AAR) was 147 and 141 per 100,000 in males and females respectively. Highest incidence rate of childhood cancer has been noticed in Delhi. Most common cancer in men and women were lung and breast with AAR of 10.5 and 27.8 respectively. HBCRs in North India reported 1,64,249 cases between 2012-2016, out of which Medanta Gurugram contributed 7,724 cases.
The cancer incidence rate for male population ranges from 269.4 in Aizawl district (highest in India) to 39.5 in Osmanabad & Beed district per 1,00,000 population. Similarly, the cancer incidence rate for women population ranges from 219.8 in Papumpare district to 49.4 in Osmanabad & Beed district per 100,000 population.
Cancers related to use of any form of tobacco were highest in the north-eastern region of the country and in higher proportions in men. Cancer of lung, mouth, stomach and oesophagus were the most common cancers among men. Cancer of breast and cervix uteri were the most common cancers among women. A significant increase in the incidence rates of breast cancer in women, and lung and head & neck cancers in both men and women was observed in most of the registries. However, a declining trend was seen in most of the registries for cancer of the cervix.
Cancer lung is mostly present with distant metastasis while cancers of head & neck, stomach, breast and cervix were present as loco-regional disease.
Read more: https://ncdirindia.org/All_Reports/Report_2020/default.aspx
(With inputs from Dr Deepak Gupta)
medanta.org/dr-tejinder-kataria/






