THE EXCHANGE | Newsletter September 2019
Opportunistic Infection in Renal Transplant Patients
Renal transplant recipients are at risk of multiple infections in view of the immunosuppressed state and background comorbidities. The microorganisms involved are frequently unique to this population and often resistant to the usual antimicrobials in view of the past history of multiple exposures and indiscriminate use of these drugs. Diagnosis in such cases is also challenging and various invasive investigations may be required for the same. These may be risky at times but make a significant difference between life and death decisions in these patients. It also spares them the various side effects associated with unjustified use of continuing empirical treatment with multiple antimicrobials. Following is the case of a renal transplant recipient who had polymicrobial and resistant infection, requiring invasive procedures to make appropriate diagnosis. The patient went on to have a successful outcome despite all odds and complications associated with invasive investigations.
Case Study
A 31-year-old male, known case of hypertension and chronic kidney disease (CKD), underwent live related renal transplant with his mother as donor in October 2011. Thymoglobulin induction was given and maintenance immunosuppression consisted of tacrolimus and mycophenolate mofetil (MMF) (steroid free protocol). He received regular post-transplant prophylaxis of co-trimoxazole for six months and valgancyclovir for three months as well. Minimum serum creatinine achieved in the post-transplant period was 1.5 mg/dl. He had an episode of acute rejection in November 2011 for which IV methylprednisolone pulses were given and he was started on oral prednisolone. His serum creatinine settled at 1.9 mg/dl but slowly crept to 3 mg/dl over the next few years.
In May 2019, the patient was admitted at another hospital with complaint of breathlessness and dry cough since 15 days and fever since one week. His investigations showed Hb- 9.5, TLC 7650 per mm3, platelet 208000 per mm3, serum creatinine of 5.6 mg/dl. HRCT chest showed diffuse ground glass haziness in bilateral lung fields. Bronchoscopy and lavage was done which was negative for regular stains of gram, ZN and KOH. All the cultures were sterile. He received antibiotics piperacillin tazobactam and levofloxacin. In view of his deteriorating clinical condition, he was shifted to Medanta - The Medicity.
The patient was tachycardic, tachypneic and hypoxic. There was pallor and bilateral crepitations. Investigations showed Hb- 9.8 gm/dl, TLC – 8560 per mm3, platelets 196000 per mm3, serum creatinine 4.9 mg/dl. Liver function tests and coagulation parameters were normal. Chest x-ray showed bilateral infiltrates. Blood and urine cultures, and H1N1 swab were sent. 2-D ECHO was normal. He was started on empirical IV antibiotics meropenem and levofloxacin. Oral co-trimoxazole and oseltamivir were added as well. In view of severe infection, immunosuppressive medications MMF and tacrolimus were stopped and oral steroid was switched to IV hydrocortisone.
After initial clinical improvement over the next 48 hours, his condition started to deteriorate again and hypoxia worsened. CT pulmonary angiogram ruled out pulmonary embolism but revealed bilateral basal consolidation with extensive ground glassing (Figure 1). IV amphotericin B was added.
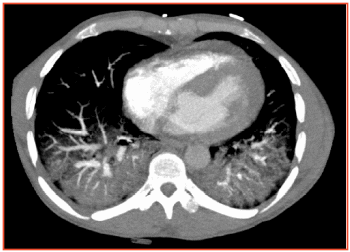
Figure 1 CT chest showing bilateral lower lobe consolidation
Bronchoscopy and lavage was done. Stains (gram/ZN/KOH) and Gene Xpert in lavage fluid were negative and cultures came sterile. BAL fluid showed positivity for pneumocystis jirovecii by immunofluorescence (IF) (Figure 2A).
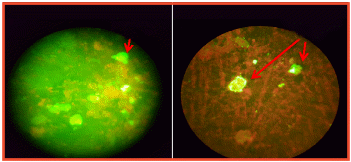
Figure 2 IF staining of (A) bronchioalveolar lavage and (B) lung biopsy showing pneumocystis jirovecii
Oral co-trimoxazole was switched to IV. Since the patient had persistent clinical deterioration, right lung biopsy was done. He developed pneumothorax post-biopsy and required intubation and intercostal drain placement. Metabolic acidosis worsened and urine output reduced, requiring initiation of hemodialysis. Meanwhile lung biopsy also showed IF positivity for pneumocystis jirovecii (Figure 2B) and the tissue culture grew enterococcus faecium and candida parapsilosis. IV Teicoplanin was added and anti-fungal was switched from amphotericin B to anidulafungin. Blood sent for CMV DNA PCR showed significant viremia (13560 copies per ml) and he was started on IV gancyclovir for the same.
As there was no clinical improvement despite the above-mentioned efforts, resistant pneumocystis jirovecii infection was suspected, and clindamycin and primaquine were added. He now required high ventilator support and developed hypercarbia. Continuous renal replacement therapy (CRRT) and extracorporeal CO2 removal (ECCO2R) were started for this.
Over the next few days, the patient started showing signs of recovery and ventilatory parameters improved. ECCO2R was stopped and he was subsequently decannulated. ICD was removed. Urine output also improved and hence dialysis was stopped. Aggressive nutrition, physiotherapy and other supportive therapies continued. He was switched to oral co-trimoxazole prophylaxis on discharge. Slowly his serum creatinine improved to 3.8 mg/dl during OPD visits and nutritional status as well as general condition also improved.
In Conclusion
Infections in renal transplant recipients can be frequently polymicrobial. Every effort should be made to arrive at a diagnosis even if it entails doing invasive procedures. Although these procedures may be risky at times and fraught with the risk of complications, it is important to guide targeted therapy so that unnecessary prolonged empirical therapy with multiple antibiotics, antifungal, antivirals etc. can be avoided. Injudicious use of these antimicrobials causes unnecessary toxicity, adds to the overall treatment cost and increases the chances of treatment resistance in future as well. In the above case, despite having a diagnosis of pneumocystis jirovecii on BAL, lung biopsy was done. And although the patient developed complication of pneumothorax requiring ICD placement, the lung biopsy led to additional appropriate diagnosis of enterococcus faecium and candida parapsilosis, thereby changing the line of treatment, and ultimately helped in saving the patient's life.
Additionally, if the patient is not showing clinical improvement, a resistant infection should be suspected and antimicrobials should be changed accordingly. In this case, the patient did not show any significant improvement in the clinical status and lung condition despite ten days of cotrimoxazole (initially oral and then intravenous) for pneumocystis jirovecii pneumonia. Hence, suspecting resistance, clindamycin and primaquine were added and the patient ultimately responded to these.
Finally, managing such patients is complex and requires inputs from various specialists. Hence, a multi-disciplinary care approach and advanced critical care support is mandatory to save lives. This patient required advanced life support measures like ventilation, CRRT, ECOO2R and was regularly monitored by a multi-specialty team comprising of pulmonologist, critical care experts, and infectious disease specialists, and had significant inputs from the microbiology and pathology departments as well. The approach was critical to a successful final outcome.
https://www.medanta.org/dr-vijay-kher/
Creatine Overuse by Body Builders
Supplement abuse is rampant in the fitness world. Enthusiasts often take them without consulting medical professionals and suffer the consequences later. Relevant scientific studies clearly warn about harmful effects of supplements such as creatine on kidneys of even healthy youth. Creatine is often prescribed by gym trainers for building muscular body alongside physical workouts in gymnasiums. Doctors get baffled seeing otherwise healthy, young males hospitalized for avoidable emergencies, brought about by unregulated creatine use without medical supervision and monitoring.
Increasing the body pool of creatine enhances its concentration in serum and also urinary excretion rate. The main metabolic waste product of creatine is creatinine, which is metabolized further to form methylguanidine. Both creatinine and methylguanidine have been implicated in kidney toxicity.
Dehydration due to excessive sweating during gym workouts, poor rehydration, along with pain killer consumption to soothe muscle ache after workouts further add to kidney damage.
Case Studies
Three such cases of kidney injury associated with creatine overuse in healthy urban males pursuing gym workouts have been reported in Medanta - The Medicity over the past ten months.
Case I The first case was that of a young, healthy, 26-year-old male, unaware of his single functional kidney, who experienced a sudden shut down of kidney (decrease in glomerular filtration rate), after abusive consumption of creatine powder for a month for body building. The patient was well-built, with bulging biceps and back muscles, and weighed 60 kg. He reported to Medanta Emergency from another hospital with complaints of shortness of breath and altered behavior since two days. In the other facility, he had been admitted and treated for anxiety disorder. Otherwise healthy with no history of past illness, he was unaware of his single functional kidney, and consumed excessive creatine supplements for body building alongside lots of vigorous exercise without proper hydration. Consequently, he developed kidney injury. Timely intervention saved his life but the condition necessitated life-long dialysis. His kidney was damaged irreversibly and will never return to its normal functioning despite best medical care.
Case II This case involved acute kidney injury in a healthy, young male wrestler following creatine abuse. This professional, state-level wrestler was hospitalized in Medanta complaining of dark colored urine associated with high dose of creatine. Following long-term, regular (two months) consumption of creatine for muscle gain, he required urgent dialysis. Further examination revealed that the reason behind the severe condition of this seemingly healthy individual was the health supplements he had been taking for the last four months on the advice of his gym trainer. Fortunately, this patient recovered and was able to participate in his tournament, as his kidney function resolved after discontinuing creatine intake.
Case III Another case of limb vessel blockage in a healthy urban male reported with pain and bluish discoloration of right lower limb associated with high dose of creatine alongside intense gym workout for one year. On investigation, his limb vessels were found to be choked, causing gangrene of lower limbs. In order to save his life, vascular surgeon had to amputate both his legs. The
patient was discharged after 26 days of hospitalization in stable condition with limb prosthesis to allow him to walk with support.
To market and promote commercial creatine supplements, its manufacturers have supported creatine drug trials to arrive at favorable position statements. Their promoters have also published some studies in favor of nil side effects of creatine on kidney (Kreider et al, 2017), which can't be relied upon.

The Food & Drug Agency (FDA) of the United States warns that consuming creatine dosages greater than 2 g/day is potentially harmful to the kidneys. Creatine is prescribed and sold in powder or liquid form by gym trainers, sometimes more than 10 g/day, without any written prescription.
Thus, better understanding of safety of creatine use and risk of kidney injury is important, and requires more double blind clinical trial, to save the lives of youth seeking body building supplements, especially for professional sports. Since the World Anti-Doping Agency is yet to ban creatine, not surprisingly, there is a high prevalence of doping (77.8%) among competitive body builders.
In conclusion, creatine in high dose, if consumed over long-term, can adversely affect kidney function in healthy individuals engaging in intense physical exercises, causing excessive water loss due to sweating, resulting in dehydration.
Creatine use in individuals with history of pre-existing kidney disease or an increased risk should be restricted, and every individual engaging in bodybuilding should undergo preventive health check-up including kidney function tests, urine tests and kidney ultrasound as a precautionary measure. Individuals consuming creatine supplement should be monitored regularly with creatine phosphokinase assay, blood gas and electrolyte tests under medical supervision to avoid acute kidney injury.
https://www.medanta.org/dr-yatin-mehta/






