THE EXCHANGE | Newsletter October 2019
Endovascular Aneurysm Repair
Technology and Precision Save Lives
Abdominal Aortic Aneurysm
Bulging or ballooning of a weakened area of a blood vessel is referred to as aneurysm. The wall of aorta can become weak due to age, disease or trauma. This may cause the aortic wall to bulge, leading to an Abdominal Aortic Aneurysm (AAA). As the bulge grows, the wall of the aorta becomes weaker. This may cause the aorta to rupture and lead to massive internal bleeding. An aneurysm rupture can cause death and needs immediate medical attention.
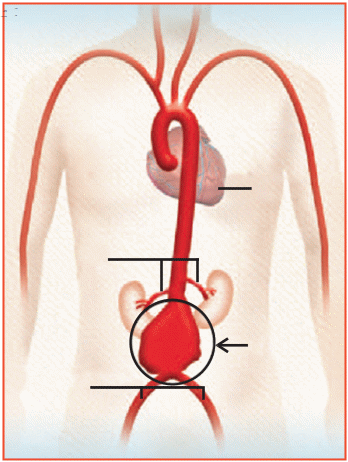
Causes
The risk of developing an AAA increases with age. It usually affects people over 50 years of age and is more common in men. Other risks include smoking and high blood pressure.
A patient with a family history of AAA is at higher risk and should consult a doctor immediately if they experience any symptom.
Symptoms
In most cases, patients have no symptoms of an AAA. However, some may experience pain in the abdomen, back or chest. Some patients might feel the aneurysm as a throbbing mass in their abdomen. An AAA is often discovered during an examination being done for other unrelated health reasons, and is felt as a bulge or pulsation (throbbing) in the abdomen. Most often, aneurysms are found during a medical test such as a CT scan or ultrasound.
Treatment Options
Open Surgery
In this treatment option, the aorta is repaired by making a large cut in the abdomen. The aneurysm section of the aorta is removed and replaced with a fabric graft. Open surgery is performed under general anaesthesia. It takes about three to four hours to complete. Patients typically spend one to two days in an intensive care unit and have a hospital stay of about a week. Complete recovery may require two to three months.
Endovascular Stent Grafting
This is a minimally invasive procedure. A stent graft (such as the abdominal stent graft) is placed inside the aneurysm without surgically opening the tissue surrounding it.
The stent graft is a fabric tube supported by a metal framework. This procedure is performed under local, regional or general anaesthesia.
It takes about one hour to complete. Patients typically don't need to spend any time in the intensive care unit and have a hospital stay of one to two days.
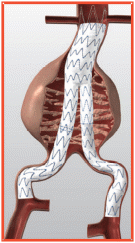
Benefits
Abdominal stent graft procedure offers the following benefits:
- This minimally invasive 'keyhole' surgery is performed through a small hole in the groin, instead of a large incision across the abdomen made in traditional surgery.
- The procedure can be performed under local anaesthesia.
- Surgical complication rate is low.
- Blood loss is less, reducing the risk of blood transfusion.
- No intensive care is required. The hospital stay is very short.
Risks
While no procedure is 100% safe, endovascular aneurysm repair is usually safer than a conventional open aneurysm repair.
Case Study
An 80-year-old man was airlifted from Amritsar for complaint of low haemoglobin (4 gm %), hypotension, and persistent anaemia despite repeated transfusions.
The patient was attended in the emergency ward at
Medanta - The Medicity. The patient was post CABG with history of open surgical abdominal aortic aneurysm repair, post splenic artery embolisation, post-cholecystectomy, hernia repair, with diabetes mellitus and hypertension.
Upon evaluation, the patient was found to have a leaking iliac artery aneurysm and aneurysm of the splenic artery eroding into the gastric wall.
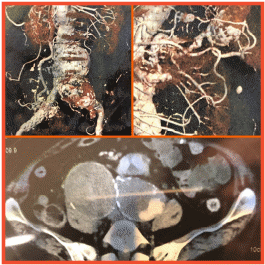
The patient was taken up for endovascular repair of aneurysm, wherein iliac aneurysm was excluded using covered stent graft; splenic artery aneurysm could not be approached in antegrade manner due to previous embolization of splenic artery.
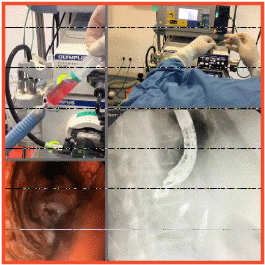
Patient was quickly shifted to endoscopy suite and the splenic artery aneurysm was approached by puncturing the posterior wall of stomach. Angiography was performed and embolization of splenic aneurysm was done using coil and glue.
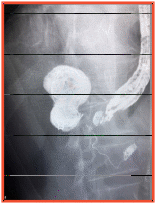
Postoperatively, the patient was observed for fall in haemoglobin and hemodynamic stability, and was found to have stable haemoglobin and vitals. Postoperative imaging confirmed complete exclusion of aneurysm with no leak.
https://www.medanta.org/dr-tarun-grover/
Surgery Offers Hope to Chronic, Long-Standing and Drug-Resistant Epilepsy
Epilepsy is a central nervous system (neurological) disorder in which brain activity becomes abnormal. Such abnormal electrical activity in the brain network causes seizures (jerks in the body) or periods of unusual behaviour, sensations, and sometimes loss of awareness.
Anyone can develop epilepsy. The disease affects both men and women of all races, ethnicity and ages.
Seizure symptoms can vary widely. Some people with epilepsy simply stare blankly for a few seconds during a seizure, while others repeatedly twitch their arms or legs. However, a single seizure episode does not imply epilepsy. Two unprovoked seizures are generally regarded a confirmatory sign of epilepsy.
Majority of patients respond to anti-epileptic medication. However, 15-20% patients do not respond to the medicines at all. In such chronic, long-standing and drug-resistant cases of epilepsy, surgery is the last and the best option. Epilepsy surgery is a procedure that removes or alters the specific area of the brain in which seizures originate. Surgery is not indicated in cases in which the seizures are well-controlled or so infrequent that they are not disabling. Disability, thus, is the most important factor that determines whether a patient is a surgery candidate or not.
Outcome of epilepsy surgery to a large extent depends on the pre-surgery work up which includes detailed clinical history of the patient, epilepsy protocol high resolution MRI, video EEG and psychological evaluation of the patient. The work-up and surgery is a well-orchestrated team work between neurologist, neurosurgeon, neuro radiologist, neuro technologist, neuro psychologist, neuro psychiatrist, neuro pathologist and trained nursing staff for patient counselling.
Epilepsy patients are mostly apprehensive about surgery for the fear of paralysis and life loss. In fact, earlier, epilepsy surgeries used to fail because of lack of advanced techniques which could pinpoint the specific area of brain responsible for epilepsy. However with advancement in technology and epilepsy surgery evolving as a niche neurosurgery skill, the procedure is very safe with a risk of less than 5%, with a success rate of about 80-90%.
Case Studies
A teenager suffering from epilepsy for the last five years with two-three seizures in a week was referred to Medanta - The Medicity. The patient used to become blank like a statue and wouldn't be able to respond for about one-two minutes. Though the attacks were not severe, the patient ran the risk of loss of control in an emergency situation such as, while crossing the road. This imposed significant restrictions and affected his social life and academic performance. Multiple anti-epileptic medicines were tried, but to no avail. Upon detailed evaluation at Medanta, we found an abnormal point in his brain at left temporal lobe (mesial temporal sclerosis).
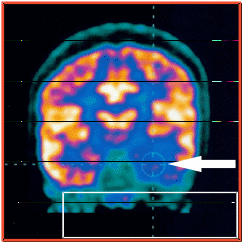
PET Scan Arrow showing abnormal point of the brain responsible for epilepsy.
His habitual attacks were recorded through a video EEG which confirmed that his seizures were originating from the same point as indicated by the MRI. The patient was operated and the abnormal point in the brain was removed. The patient continues to be seizure and medication free. Now a confident individual, the patient is attending university and drives confidently as he does other normal life activities.
Another patient, a medical student, had been suffering from seizures for seven years. Despite being on five medicines, her situation was not improving. The girl was evaluated as part of the pre-operative work up, and it was found that her abnormal point was sitting right over the anatomical possible speech control area in the brain (Broca's). The patient was operated with a special technique known as awake craniotomy. This is an awake procedure, in which the patient is only given local anaesthesia on the scalp. She continued to speak through the surgery. The patient is now seizure-free, and leading normal life.
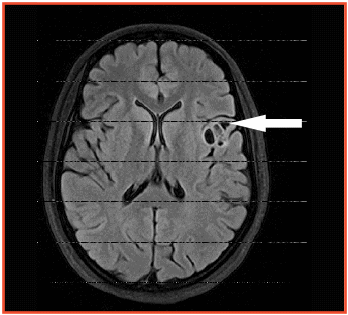
MRI Arrow pointing to an abnormal area in the brain causing epilepsy. This area is our anatomical speech area (Broca's)
https://www.medanta.org/dr-atma-ram-bansal/






