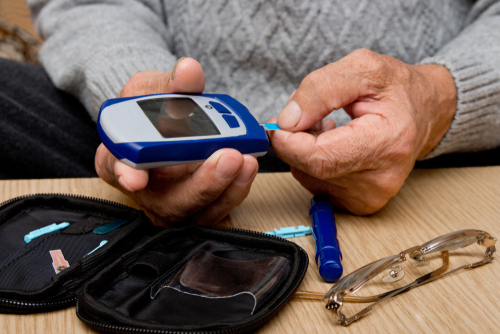
Ageing and Diabetes
In 2016, the World Health Organization compiled a report titled “Global Report On Diabetes” that stated, over 422 million people the world over suffer from diabetes. This number had quadrupled since 1980.
Today, people have the opportunity to live longer than ever before. This long life however, is often accompanied with a host of illnesses, diabetes being one of them.
A person is said to have diabetes when the pancreas either fail to produce a hormone called insulin (known as type 1 diabetes) or when the pancreas produces the insulin but it is either not enough, or the body is unable to utilize it (known as type 2 diabetes).
When food is digested, it is converted into glucose. Insulin moves glucose into cells, where it then produces energy. However, a person with diabetes is unable to break down glucose into energy. This inability causes blood sugar levels to rise above what is considered ‘normal’ levels.
Ageing and Diabetes
While everyone with diabetes requires life-long management and care, dealing with diabetes in old age has its own set of challenges. As one ages, the body begins to develop insulin resistance; the fat and muscle cells do not respond well to insulin and so cannot easily absorb glucose from the bloodstream. As a result, the body needs higher levels of insulin to help glucose enter the cells. The pancreas creates this excess insulin initially, but as one gets older, they begin weakening, causing dysfunction. In addition, there is a decline in the number of beta cells of the pancreas which are the insulin-producing cells. For senior citizens other challenges include frailty, physical dependence, multiple medications and presence of other health conditions like arthritis, high blood pressure, or weakened bones that have their own treatment plans. All of this means diabetes management becomes tougher as one ages.
Although diabetes is a disease linked to high blood sugar, having low blood sugar can be serious for the senior citizens as well. Hypoglycaemia or low blood sugar occurs when insulin clears the glucose from the bloodstream fast, leading to a sharp drop in blood sugar levels. This drop can be caused due to certain medications, irregular meal timings, over- exercising, a significant gap between eating and taking the relevant medication, as well as other diseases. When blood sugar levels fall too low, it increases the risk of cognitive decline and other major adverse outcomes like seizures, coma and even death. Some symptoms of hypoglycemia like fatigue, irregular heartbeat (arrhythmias) and sweating may remain unreported and untreated.

Detection Remains a Challenge
One of the key challenges in identifying diabetes amongst senior citizens is the presenting symptoms. The classic signs of diabetes are polyuria (increased urge to urinate), polydipsia (increased thirst), and polyphagia (increased hunger), but often senior citizens may not exhibit these. Only when over a period of time the high blood sugar levels remain untreated, they might demonstrate an increased urge to urinate and drink water. Symptoms of the disease in senior citizens may include body aches, pain in the abdomen and calves, weight loss, recurrent infection and severe dehydration. Some women-specific symptoms are urinary tract infections or fungal infection in the genitals. In young people, diabetes comes with the classic signs along with fatigue, blurred vision, nausea, and slow healing of wounds.
Complications of Diabetes
Retinopathy
High blood sugar levels damage the back of the eye, the retina, and can cause blindness if left undiagnosed and untreated.
Nephropathy
Diabetic nephropathy is a serious kidney-related complication of diabetes. It affects the ability of the kidneys to do their usual work of removing waste products and extra fluid from the body.
Neuropathy
High blood sugar levels can cause damage to the nerves and interfere with nerve functioning; these then cause diseases in other organs.
Cardiovascular diseases
When it affects the cardiovascular system, neuropathy can cause heart attack, arrhythmias, and raised blood pressure levels during exercise.
Stomach ailments
When the nerves controlling the stomach are affected, a condition known as diabetic gastroparesis may result. In this condition, the movement of food through the stomach is slowed or even stopped, which can cause nausea and vomiting.
Bladder
Neuropathy can affect the bladder, making it difficult to tell when it is full, sometimes leading to urinary incontinence.
Managing Diabetes
Treatment of diabetes with drugs in the elderly has to be individualized based on the health condition of the patient, prevailing glycaemic control (levels of blood sugar) and other comorbidities (presence of one or more diseases). Lifestyle modifications along with oral drugs and insulin therapy are ways in which doctors keep blood glucose levels in check.
Metformin remains the first line therapy for most patients, the doctor may prescribe other glucose lowering medications as well. Insulin therapy involves administering insulin in the fat under the skin using a syringe, insulin pen or insulin pump when the pancreas are not producing enough. Some patients require both oral medications and insulin therapy.
Having other conditions makes managing diabetes tougher, especially if those health issues have their own treatment regimes. Drug interactions in the body when multiple drugs are being used has the greatest impact in an ageing body. Treatment plans for senior citizens therefore need to be monitored very strictly and regular communication between the patient and the doctor is imperative.
Living with Diabetes

Exercise
Exercising regularly helps the muscles become more sensitive to insulin. Senior citizens can engage in simple physical activities like walking and yoga.
Eat well
Eating well can help manage blood sugar levels. A diabetes patient should eat a balanced diet that includes fruits and vegetables, protein, whole grains, cereals and dairy products.
Medicines
Medicines are a critical part of diabetes treatment and should be taken on time and in the right dosage. It is advised to regularly consult with the doctor for periodic adjustments in the dose and frequency of medications, based on the blood glucose readings and other laboratory parameters.
Regular health checks
A diabetic should make it a point to go for regular health checks to detect any risk of diabetes-related health complications.
Monitor blood sugar levels regularly
Self-monitoring in diabetes is essential to understand how food intake, physical activities and medication dosage impacts the blood sugar levels.

